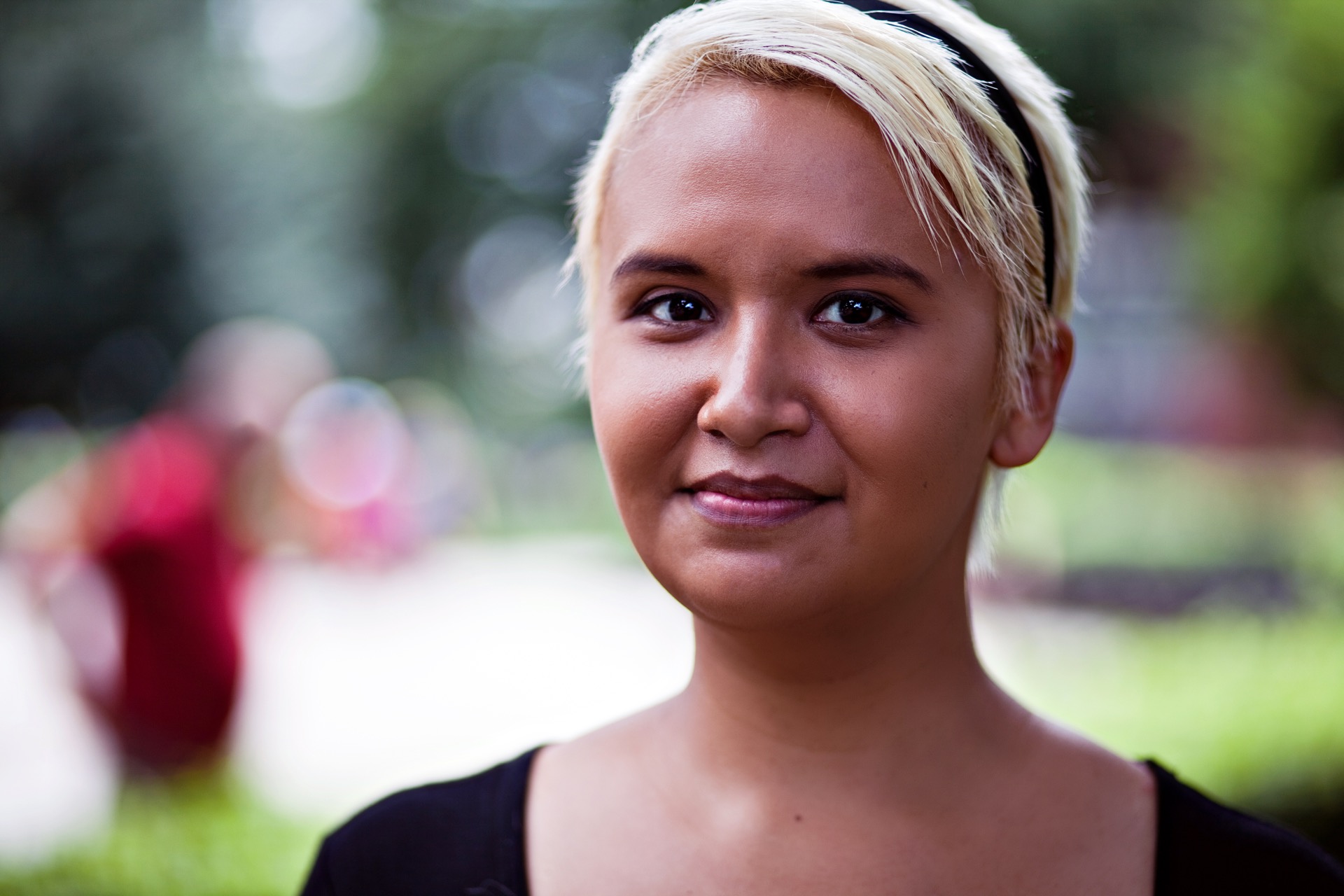
Anita Estrada
is a suicide attempt survivor."I survived a suicide attempt."
Anita Estrada was a 31 year old nursing assistant and student when I interviewed her in Washington, DC, on 6/23/13.
I really didn’t realize it until recently, but I’ve kind of always been suicidal, even since I was a child.
I never attempted suicide. I never planned anything, but I remember being like, ‘Well, I really hope I just go to sleep and not wake up,’ kind of thing. I was raised in a very Christian household and suicide was a sin and all that, so I never really told anyone. My mom was a single mother raising me and my siblings by herself so I didn’t want to be presenting another problem for her to have to fix.
It really became more obvious, more of an issue, when I got in my late teens and early 20’s—the depression. I was diagnosed with depression when I was in my early 20’s—depression with atypical anxiety—and then when I had my first suicide attempt, they changed it to bipolar disorder. I’m like, ‘Well, that explains all the racing thoughts and all that.’ I would spend money I didn’t have. I had these all these ideas and they never…it was the mania. I just never really knew what was going on, so I couldn’t control it. My first suicide attempt—I guess that was in 2005, so I was 24. I attempted suicide again in 2008 which, at that time, was awkward because I was working at a hospital in the ICU, and that was the same ICU where I was treated.
Some of the comments that people made…my coworkers just made me mad. But I was so mad I didn’t want to say anything…
[They were] talking about people that they knew who said they were gonna [attempt] suicide: “Oh, it was just for attention,” this and that.
I’m like, “Well, I’m pretty sure, at the time, I wanted to die, so I’m not sure how your friend really fits into this conversation. If I really wanted attention, I would have done something else, not try to kill myself.”
It was just kind of sad. Some of the nurses I worked with would make comments about some of the patients that we got in who were suicide attempts. They’d say, “Why don’t we just let them die?” and stuff like that, and they didn’t realize that [I had a] history with depression and all that.
There’s just kind of this ignorance. Either they don’t really care to know, or they were just not informed about mental health and mental illness. They just think that a person who attempts suicide is not worth the time to take care of.
I wouldn’t say the same thing about someone who had a heart attack. Even if they ate twenty cheeseburgers every day for their entire life, I wouldn’t say, “Oh, let ‘em die. They don’t know how to take care of themselves.”
It was disturbing to me to see someone who is supposed to be a medical professional make comments like that.
My last suicide attempt was in 2011, and that was really bad. [I guess it was just societal pressure.] People on medication are somehow lesser or whatever. I didn’t want to be on medication for the rest of my life, so I tried against my doctor’s orders to wean myself off. I stopped eating and I stopped sleeping, and then I tried to kill myself. It was really bad because I was on a ventilator for a few days, and I was in the hospital for almost two weeks. But it’s really weird. Something changed and I don’t know what. When I was first released from the hospital, I was really intent on trying to kill myself again. I was like, ‘Well, I don’t have any pills, I don’t have a gun, but I’m gonna see if there’s another way.’
When I started medication and therapy again, it changed and I felt better. It was just a lot different than before, than the other medications I tried. They try everything with you—Effexor and Seroquel and Abilify and Zoloft and all this other stuff. I don’t know if maybe it’s ‘cause I finally found some sort of purpose where I felt like there was an attainable goal, ‘cause before I felt kind of lost. I was studying art, but I always kind of felt like I wanted to do something to help other people. When I finally decided to try to become a nurse, it just felt right.
I think maybe the medication probably had a lot to do with it. I think it synced, making that decision and also being on the medication. At least, it helped me…deciding to not [die by] suicide and to work on being a nurse and helping other people—contributing to good, rather than contributing to all the bad things, ‘cause there’s so much bad stuff. I just can’t watch the news. I can’t think about any of it.
I’ll be like, “This is just gonna bring me down and I’m just gonna be in one of those moods where I just cry,”
And people are gonna be like, “What the hell is wrong with you?”
And I’m like, “But, but!”’
I get mad at people for not caring. The most I can do is try to help in my own little way.
So, if I fail as a nurse, I’ll be a mime. I don’t know. I’ll move out on the street in a cardboard box and just be a mime. I’ll be a street performer.
Des: Something that really interests me is the way you talk about the medical profession and the way that you said people who attempt suicide are treated.
Anita: I think, unfortunately, it varies from nurse to nurse. I think it has a lot to do with that nurse’s personal experience with mental health and mental illness. You’ll meet nurses who have family who have have been diagnosed with bipolar disorder, depression, schizophrenia, and they have some understanding of how to work with people. Then there are some nurses who don’t care, and I guess it affects how they treat all patients. The nurses who’ve made those comments are kind of dismissive with a lot of other patients, too. Some medical professionals, they’re just there to earn a paycheck and some people actually get into it because they’re interested in helping and getting a person back to their healthiest state…
Nurses are overworked. Psych, as far as education, is only—in my program—a seven and a half week course. That’s it. If you consider everything else—acute care, elderly care, pediatrics, OB/GYN—psych doesn’t get much time dedicated to it, unless you do extra training in addition to your degree. I think it takes a certain type of person to really take the time to understand people with mental health disorders because it doesn’t present itself like any other physical disorder, although it always seemed curious to me that we wouldn’t treat mental health the same as we’d treat the rest of the body. The brain is part of the body.
You can’t just completely cut off your brain and be like, “Well, we’ll just treat this… the rest of this? You’re fine.”
It’s all interdependent. I think that’s what’s the most frustrating about working with people in the medical field who don’t take the time to address mental health issues, because it’s part of your physical health. It’s not just some emotional thing you get over.
One of my pet peeves is how people will talk about suicide being a ‘permanent solution to a temporary problem.’
I’m like, “Fuck that! I’m gonna have bipolar disorder for the rest of my life. It is not a temporary problem.”
The issue is that I have to get to know myself enough to control those ups and downs. When it came to my depression and suicidal ideations, it hit me like a tornado, and the best I could do was survive it. It wasn’t a matter of staving it off. It was just making sure I didn’t hurt myself…
That was always a pet peeve of mine. ‘It’s a permanent solution to a temporary problem.’
I’m like, “Well, you deal with this and tell me it’s a temporary problem. I’m not doing this because some boy broke my heart or I just wanted someone to talk to. No, I did this because I didn’t really think I had an option…”
It bothers me, because I’m on medication. I’m on Depakote and long-term affects are not good. The chances are that I will have to deal with some side effects that are permanent. How do you balance that out with dealing with your current issues if you’re not on medication? If I’m not on medication, like I said the last time, I stopped eating and I stopped sleeping and then I tried to kill myself.
Des: [I’m noticing you have a lot of scars on your arms.] How do you feel about people asking you about them? Are you honest? What do you say?
Anita: The truth is, I’ll notice people looking at them and then quickly looking away. No one’s ever come right out and asked me.
I remember someone—a patient I was helping while I worked at the hospital—she made a comment about a past mistake or something. If they were to ask me, I’d have to be honest. I mean, what am I gonna tell them? I got in a fight with a bear? That’s the only way I would have gotten something like that.
I sometimes feel like coming right out and explaining it, but I feel like, if they really want to know, they should ask when they’re comfortable. The people I’m closest to know what they’re from. People who don’t know…I’m not really interested in disclosing my dirty laundry to everyone.
If it were someone who I thought could maybe relate, I’d talk about it, or for someone who self-injury was a problem, I’d be like, ‘Hey, you know what? I understand where you’re coming from.’
I think, for the most part, people are just like, ‘Eh,’ ‘cause no one ever asks me about it.
Des: I interviewed a man who struggles with self-injury recently, and he said that he kind of wished that people would ask.
Anita: I kind of do, because I know you notice them. You just looked at my arm. You would ask me about any other scar on my body, you know? I had a scar right here on my forehead that people would always ask about when I had my hair pulled back.
Maybe if people were more open about it, we’d be more comfortable talking about things like self-injury and the people who felt like harming themselves or thinking about suicide would feel more comfortable being like, ‘Hey, can I talk to you?’
I’d be like, ‘Sure.’
It’s a dirty secret kind of thing. Everyone knows, but no one talks about it.
Des: Do you feel ashamed of your scars at all? How do you feel about them?
Anita: At first I did. I was scared of wearing short-sleeved shirts to work, which is pretty damn impossible, considering how hot it gets in this area during the summer. I noticed that, when I would walk and stand, it was always with my arm against my stomach or behind my back.
I guess, with time, it just became like, ‘Well, you know what? They’re there and if anyone has a question about them, they can just ask.’
Des: Maybe I didn’t ask the right question. How do they make you feel when you see them?
Anita: Regret, maybe. That would be the best answer. Just regret that I wasn’t in a state of mind where I could personally feel like I was worth someone else’s time who could take care of me or help me. For the longest time, I wouldn’t talk to anyone about being upset.
Time passes and it’s just like, ‘Well, they’re a part of my history now, along with my appendectomy scar and my thoracotomy scars.’
It’s just one of things.
Des: How do you feel about self-injury? Is it a suicidal act or is it coping?
Anita: Self-injury, for me, was always a coping thing. Whenever I injured myself, it was more me just trying to deal with all my [emotions]. It was a distraction. I always considered it [similar to] someone going on an alcohol binge or doing drugs or anything like that. And then it became an addiction, kind of…
It’s something I can focus on, something tangible where I can be like, ‘There is something wrong with me, ‘cause look right here. I’m bleeding and it’s not just all in my head.’
Days after, when it was sore, it would distract me from everything, and then it would kind of make me feel better because it wasn’t just my brain. I can’t reach into my brain and see what’s going on and touch it, but I could touch and see this, so it was more of a coping thing.
Des: Do you still cut yourself?
Anita: No. I think the last time I did was several months ago. I don’t remember why I was upset. I was disappointed in myself, but I just considered it a sick act.
When I was first diagnosed, I expected it to go in a pattern or in steps. I would get better and better and better. I didn’t consider that every day would be a struggle, whether I was in a horrible mood or in a good mood or this and that. Some days, you’ll just feel really crappy, and some days it won’t affect you at all.
So, I felt bad the last time I cut myself, but then I [thought], ‘There’s no point in getting down on myself about it, ‘cause it’s not gonna help anything.’
I think a lot of people have a misconception when it comes to being diagnosed with a mental illness that once you’re diagnosed, it’s all a path to getting better. No, it’s a maintenance thing. It’s every day. It’s like being a diabetic. If you were born a diabetic, you’re gonna be a diabetic every day of your life, and it’s just a matter of making sure you’re okay from moment to moment. It’s the same thing with mental illness. It’s gonna affect your life every single day, and it’s just a matter of making sure you’re the healthiest you can be, and sometimes it’s gonna suck.
Des: Is suicide still an option for you?
Anita: No idea. Like I said, it’s a day-to-day thing. The one thing I don’t want to tell anyone I love is that I will never do it again, because I don’t know if I will never do it again. I can’t tell the future. I don’t know if it’s going to get worse, if the medications are going to stop working, if my circumstances will change where I can’t afford medication and therapy. I’m lucky enough to have health care right now. A lot of people aren’t. In the past, I always thought, ‘I’m not gonna die a natural death; I’m gonna kill myself. That’s just how it’s gonna go. One of these days, I’m just gonna decide I’ve had enough, my life’s over and I’m gonna kill myself.’ Right now, I really consider a natural death to be possible in my future, but I can’t rule out that I won’t kill myself because I don’t know how it’s gonna go. I just don’t.
Rebecca’s story is sponsored by a grant from the hope & grace fund, a project of New Venture Fund in partnership with global women’s skincare brand, philosophy, inc. Thanks also to Al Smith for providing the transcription to Rebecca’s interview, and to Sara Wilcox for editing.